Most doctors retire in their mid to late 60s. The average retirement age is about 65. But retirement ages vary a lot. They depend on specialty, money, health, and job satisfaction. Some physicians leave clinical work before 60, others continue well past 70, and many shift gradually from full-time patient care into part-time, teaching, or advisory roles instead of stopping abruptly.
This guide is for physicians in the medical field who want a realistic picture of retirement age trends in the medical profession, not guesses or anecdotes. The insights here come from workforce studies, physician surveys, and specialty data. You will learn how retirement ages differ. You will see why doctors retire later than expected. You will learn how medical specialties affect retirement timing. You will also learn how to plan your medical career with lifestyle and money in mind.
Average Retirement Age for Physicians
What the Latest Data Shows About When Doctors Retire
The most reliable way to understand physician retirement is to look at population data instead of individual stories.
One large physician cohort study found the average retirement age of physicians was about 65.1 years. That figure sits close to what many doctors informally consider a “normal” retirement age, but the range around that average is wide.
Workforce age data adds another layer. Analysis shows about 30 percent of U.S. physicians are 60 or older and 23 percent are 65 or older while still in active patient care. This tells you something important. A large share of doctors are already at or beyond what the general population calls retirement age, yet they continue working in clinical roles.
Survey data also breaks down timing. The american medical association reports that around 30 percent of physicians retire between ages 60 and 65 and about 12 percent retire before age 60. That means most doctors do not retire extremely early. Early exit exists, but it is the minority.
Globally, the trend is similar. OECD workforce analysis shows the share of doctors over typical retirement ages is rising across countries, reflecting delayed exit from the profession. This is not just a U.S. pattern. It is a broader shift in the medical profession.
Industry survey data across medical specialties gives more detail. Reports show approximate average retirement ages such as primary care around 67, cardiology around 66.5, radiology around 66, anesthesiology around 66, OB GYN around 64.5, and surgery around 61 in some datasets. These are not strict rules, but they show meaningful variation by specialty.
Why does this matter to you? Because your expectations about retirement age affect your retirement plan, your savings targets, and how long your income must support your lifestyle and pension plans.
Read: [How Much Money Do Doctors Need to Retire at 50? A Realistic Breakdown]
Median vs Early and Late Retirement Among Physicians
Looking only at averages hides what life actually looks like at different retirement ages. The median age of retirement for many groups of doctors still clusters in the mid 60s, but experiences differ sharply.
Retirement timing | Typical range | What life often looks like |
Early retirement | Before 60 | Often driven by burnout, health, or strong personal finance discipline. Physicians may stop full-time patient care but still consult, teach, or do part-time work. |
Median retirement | 60 to 65 | The most common window. Doctors reduce call, cut hours, or shift roles before fully stepping away from medical practice. |
Late retirement | After 65 | Physicians continue because they enjoy work, feel a sense of duty, or want more financial security. Many move into lower intensity roles in the medical field. |
This table is not about judgment. It shows that physician retirement is usually a transition, not a single date. Many doctors never flip a switch from full speed to zero. They adjust workload, responsibility, and schedule over time.
Why Doctors Retire Earlier or Later Than Average
Physician Burnout and Workload Pressure
The medical career path is long and demanding. Years of training, emotional labor, administrative load, and high responsibility all add up. Burnout is a real driver of earlier retirement ages.
Physicians who feel exhausted by call schedules, electronic records, and constant performance pressure may choose to retire early or at least leave heavy patient care roles. Burnout also connects to patient safety. Fatigue and cognitive overload can push experienced doctors to step back when they feel they cannot maintain their own standards.
This is especially relevant for family physicians, who often manage large panels, complex chronic disease, and extensive coordination. Over decades, that workload can become physically and emotionally draining.
Financial Readiness and Retirement Savings
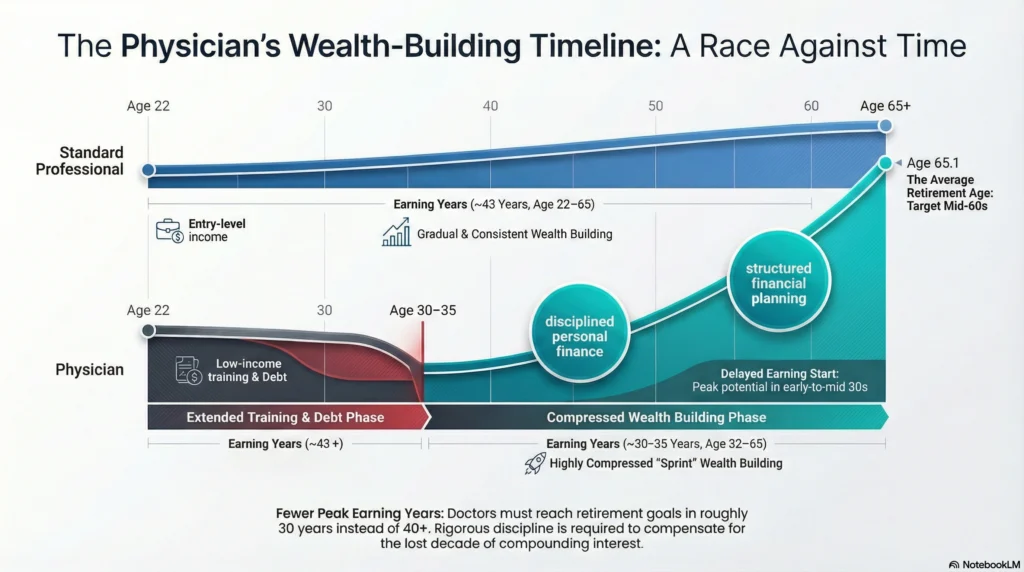
Money is the other major factor. A doctor with a clear retirement plan, strong retirement planning habits, and structured financial planning has more freedom in choosing retirement age.
Physicians start earning later because of medical school and residency. That delayed start compresses wealth building into fewer peak earning years. Some doctors compensate with disciplined personal finance, while others focus on lifestyle and catch up later.
Doctors without adequate retirement savings or pension plans often delay retirement. Those with a strong balance sheet and guidance from a financial advisor can retire on their own terms.
Read: [How Much Do Doctors Need in a 401k to Retire Comfortably?]
Health, Energy Levels, and Cognitive Demands
Medicine requires a lot of thinking and mental effort. The ability to make rapid, accurate decisions matters for patient care and patient safety. As physicians age, they honestly assess their stamina, memory, and focus.
Some reduce procedural work or night shifts. Others move into mentoring, administration, or teaching roles. Family doctors and doctors in thinking-based specialties can adjust more easily. Doctors in physically hard fields like general surgery find it harder.
Health is deeply personal. Two doctors of the same age can have very different energy and resilience, leading to different retirement ages.
Retirement Age by Medical Specialty
Surgeons and Procedure-Based Specialties
Specialties that rely on fine motor skill and physical endurance often see more variability. In some datasets, surgery shows earlier average retirement ages, partly due to the physical demands of the work. General surgery in particular requires stamina that may become harder to sustain later in life.
Still, many surgeons transition into supervisory or teaching roles rather than fully leaving the medical profession.
Emergency Medicine Physicians
Emergency medicine combines shift work, high acuity, and stress. That environment can push physicians toward earlier retirement or reduced hours. Some move into urgent care, administration, or nonclinical roles to extend their medical career without the same intensity.
Primary Care Doctors
Family physicians and other primary care doctors often build long relationships with patients. That continuity can be fulfilling, which encourages some to work longer. At the same time, large patient loads and documentation burdens can accelerate burnout. This push and pull helps explain why family physicians show a spread across retirement ages.
How Doctors Know It’s Time to Retire
Professional, Personal, and Family Considerations
Doctors rarely retire because of one factor alone. Most weigh several areas together.
Professional factors include satisfaction, stress level, and whether the work still feels meaningful. Personal factors include health, energy, and life goals outside medicine. Family considerations often become more important over time, including time with partners, children, or aging parents.
Financial clarity matters here too. Many doctors talk to financial advisors. They check if their retirement plans support their lifestyle. Understanding personal finance numbers, income needs, and long-term projections makes the decision less emotional and more grounded.
Read: [How Do Doctors Retire Early? What Makes It Realistic (and What Doesn’t)]
Also Check Out: [Financial Freedom Calculator for Doctors]
How a Financial Advisor Fits and When
This is where guidance should feel clarifying, not sales-driven. Over the years, we built Medicine and Money Show to fill that gap with education first.
Some doctors prefer a structured path.
If that resonates,
- 📘 Our book Freedom for Doctors offers a physician-written roadmap to financial independence, personal balance, and long-term financial security. Others want to test ideas first.
- 📥 Our free LIFTOFFNOW Physician Financial Flight Plan breaks the framework down without commitment.
- 📞 And if you want to talk through your situation, a short clarity call can help you decide next steps without pressure.
- 🎧 Listen to the audio version of this guide while commuting or between shifts
For deeper context, Read: [Student Loan Repayment Strategies for Doctors: A Clear Plan for High-Income Physicians] to see how debt fits into the bigger picture.
FAQ
The average physician retires around age 65, though many continue working past that depending on specialty, health, and financial readiness. Some retire in their early 60s while others remain in patient care into their late 60s or 70s.
No, doctors are not required to retire at 65 unless limited by employer policies, hospital bylaws, or personal health factors. Many doctors keep working past the usual retirement age. They often work in non-surgical or part-time jobs.
Yes, a doctor can retire at 45, but it requires unusually high savings, low expenses, and a deliberate early retirement strategy. It is rare and usually involves strong financial discipline, alternative income sources, or a transition out of full-time clinical work rather than a complete stop.
Physicians retire early mainly due to burnout, health issues, administrative burden, financial independence, or a desire for better work–life balance. High stress specialties and long-term workload pressure often accelerate the decision.
Some physicians retire later because they enjoy clinical work, value patient relationships, or feel a strong professional identity tied to medicine. Others delay retirement to strengthen financial security or because they started earning later after long training.





